Patient Stories

Meet Kay Mara
Kay’s story started in February 2023, when she was hospitalized with acute respiratory failure and infection in her peritoneal dialysis catheter. After presenting at the PCH Emergency Department, she was sent to QEH where her hemodialysis line was replaced. Once she was stabilized, Kay was transferred to the Surgical Restorative Unit at PCH for her recovery and rehabilitation

New Year’s Baby: A Life Hanging in the Balance
April 22, 2024
Courage, quick thinking, thorough training, and the unyielding dedication of our healthcare professionals prevented tragedy when every moment counted.
Meet April and Family
Teacher April Chaulk and her husband Brockk had been waiting nine long months for their first child to arrive. The day came last year when little Baxter joined them in the Maternal Child Care Unit at the Prince County Hospital. At first, all seemed fine. This should have been the most joyous moment of April’s life. “Shortly after Baxter was born, he was placed on my chest for about 30 minutes and then I started to feel extremely weak and the nurse came and checked and I had hemorrhaged very, very badly.” April was rushed to surgery to investigate the source of her bleeding. “I remember looking at my husband and Baxter, he was under the lights.” Baxter needed some time in the Infant Warmer (included in each of the private birthing suites), he also had a bit of jaundice that could be cleared up with UV lights, if needed (it wasn’t). “I remember leaving him and seven nurses rolled me down to the OR. I opened my eyes part way through and looked at the nurse and said, ‘am I going to be okay?’ and she said ‘We are going to get you back to your baby.’ At that … View full news story.

October 6, 2022
Walking into the Credit Union Place on September 3rd was heartwarming. It was refreshing to join our friends and neighbours once again with the shared purpose of ensuring a bright future for patients at PCH. To watch as approximately 1000 community members gathered to celebrate their hospital was inspiring. As we began to welcome speakers and guests, the mood was jubilant. And though we knew several high-profile gifts were coming to the stage, we weren’t prepared for so many surprises. Mr. Robert Irving arrived with one such gift – a $250,000 cheque!The auction itself also had a banner year, raising $83,900. This great success was due in part to the last-minute tripling of an auction item. With auction prize donors Danny and Martie Murphy on hand, auctioneer Allison Smith secured their consent to offer not one, but three of their famous “Dinner at Gingerwood” packages – meaning each of our top three bidders walked away with dinner for 18 at the Murphy estate. Approaching this 14th event, organizer and financier Warren Ellis had a grand total in mind, a long shot at $2.5 million in cash and future pledges. As the night neared its end and the dollars were tallied, … View full news story.
Vital Signs Appeal 2022
With the recent mailing of our annual Vital Signs appeal, our fundraising year is officially underway. Chief amongst the essential, life-saving medical equipment to be replaced are the hospital’s three Ultrasound machines. At $525,000, the units make up a significant portion of the $2,391,810 list of greatest needs for patient care. “Most people would recognize this Ultrasound technology for its use in obstetrical exams at all stages of pregnancy, but ultrasound is used for many things at PCH each day ranging from aneurysm detection to locating gallstones, blood clots, breast exams and vascular studies,” says Meaghan Noye, PCH Ultrasound Coordinator. “We are VERY excited to be able to get new machines! The machines that we will be getting are amazing! We will be getting some new imaging packages that allows us to expand the scope of exams that we currently perform. We will still be able to perform all exams we currently offer and when trained on the new machine capabilities, be able to offer additional information to physicians. Image quality is greatly improved on the new machines as well, which allows us to see more while improving patient comfort.” “Ultrasound can be a window into a patient’s diagnosis,” said … View full news story.

Meet Dayla and Janelle
Dayla just didn’t seem like herself. She was never a colicky 13 month old, but she had been out of sorts lately. Her mother, Janelle Gallant, chalked it up to a reaction to her recent one year inoculations. But, as the days stretched to weeks, she began to worry. That’s when Janelle took little Dayla to Western Hospital where she received blood work. Finding nothing of great concern, Janelle next visited her pediatrician who did an exam and then arranged an Ultrasound to see if the source of Dayla’s discomfort could be found. That was when every mother’s worst fear came true. It was Christmas-time, they had just put their tree up when she had that first Ultrasound. Later that day they heard from her pediatrician who told them the Ultrasound revealed a 14 cm tumour in her belly. When you consider that the average one year old girl is only 74 cms tall (29 inches) the diagnosis becomes even more unsettling. Dayla was immediately taken to the IWK where she received a major 11 hour surgery (removing one adrenal gland) followed by five rounds of chemotherapy. She also received a double bone marrow transplant in Toronto along with immunotherapy … View full news story.

Lights for Life: Meet Susan and Harleigh MacKay
November 4, 2021
We love seeing old friends come to PCH for a visit this time of year. We had the opportunity to visit with Susan Mackay when she came by PCH to make her annual Lights for Life dedication. Susan and husband Harleigh have been making gifts to Lights for Life since the very beginning in 1995. Some gifts have been to honour their grandchildren while other donations have been made in memory of loved ones they’d lost including Susan’s mother Bessie, sister Barbara, father George and father-in-law John. “Lights for Life is always a wonderful way to start off the Christmas season for us. It has become a tradition,” said Susan. Friends of PCH would likely know Susan from her many years as a nurse here at the hospital. But you may not know that Susan has also been a longtime Lights for Life committee member, staff choir conductor, and former honourary chairperson; helping to guide the event to what it has become. “I became involved in Lights for Life because PCH has always been a very important part of my life” Susan continued. “I was always so proud to say I was a RN at PCH and it was a … View full news story.
Caring Connections: Autumn 2021
The autumn edition of the Prince County Hospital Foundation’s newsletter. This issue features stories on Grass Roots and Cowboy Boots, the revamped X-Ray Room, and a feature story on the breast cancer journey of Nancy Key.

Meet Claudette
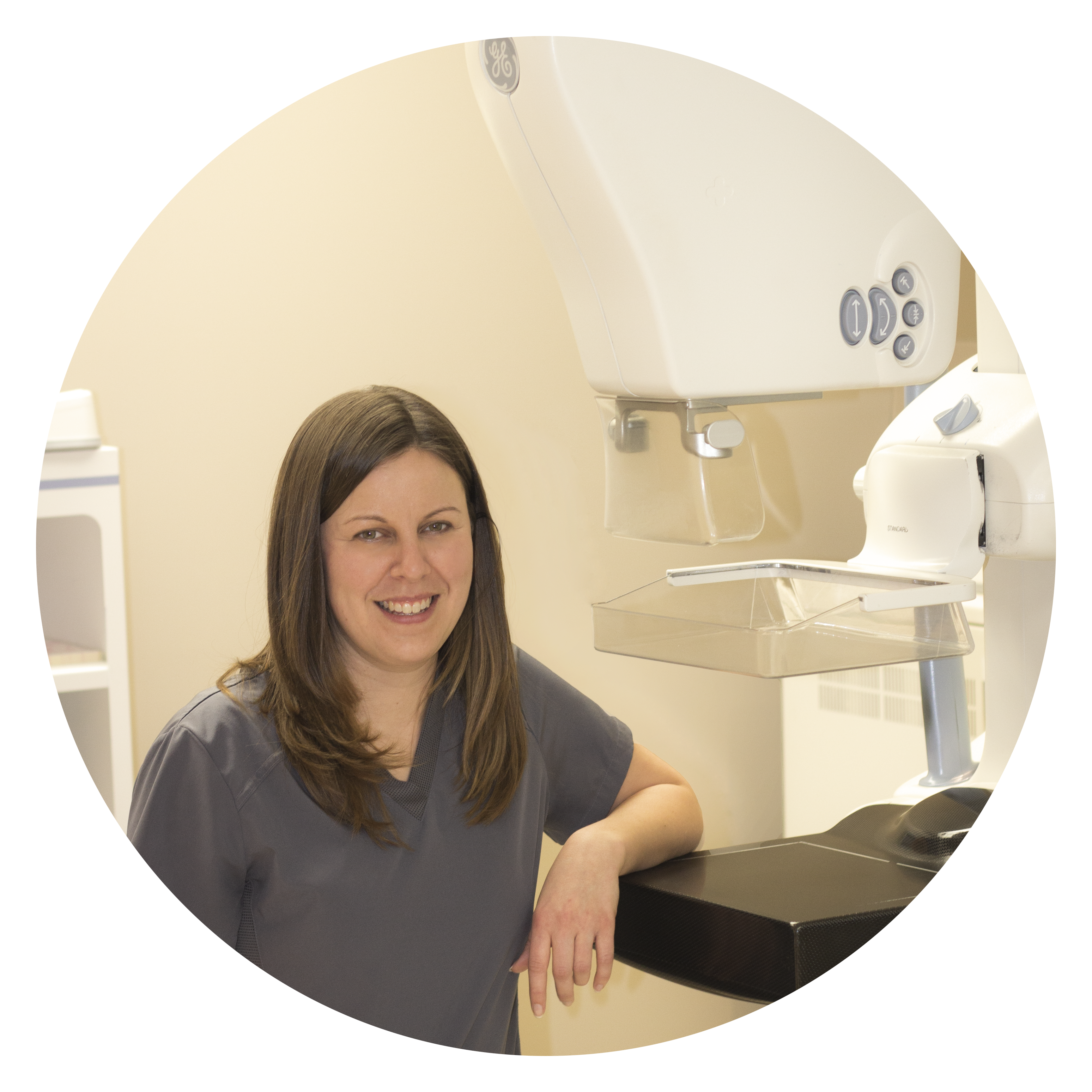
Claudette Theriault is a planner. She likes to know exactly what she is doing and when. But, there is no way to plan for breast cancer. In the late nineties, Claudette found a lump the size of a grape; it was Stage Three Breast Cancer. She had a lumpectomy followed by radiation in New Brunswick (there was no radiation on PEI at that time) and then six months of chemotherapy at the old PCH on Beattie Avenue.Every spring since then she’s gotten a mammogram. Each time her appointment came around, she was nervous her cancer had returned but knew that it was better to know than not. “It’s always a period that I’m anxious,” Claudette told us in a recent interview at PCH. “I was always afraid that I would get it again. You just wait, wait, wait for your results.”Last year the day came. Claudette’s annual mammogram was with technologist, Amy Murphy. “Amy was thorough. I thought, ‘If I have ANYTHING, she’s going to find it.’ I left there with confidence that if there was anything at all, that she would have found it. She was so thorough, compassionate, caring, and gentle.” Amy was new in her role and … View full news story.

Vital Signs 2021
The Prince County Hospital Foundation is launching their annual Vital Signs appeal this week and Digital Mammography is front and centre of the $1,788,900 campaign.

Meet Andrea
Andrea Wile is a PCH Registered Nurse, the Nurse Manager in the Maternal Child Care Unit, a small business owner in Summerside with her husband Kevin, and a member of the PCH Foundation Board of Directors. When Andrea was a teenager she lost her mother to breast cancer. Though her mother’s cancer was thought to be found early, advancements in mammography have meant that Andrea’s cancer was found even earlier…when she was 35. Andrea recounts “As scary as it is to get results and as scary as it is to get diagnosed, I’d rather know than not know. The options in front of me were positive because of early detection.”Andrea’s mother did everything that was recommended to her in the early 90s, but died from cancer seven years later. “I was blessed,” said Andrea, “because although I couldn’t ask her, my mom was a nurse and kept diaries of her health. I was lucky to be able to read it.” The path her mother walked in those diaries helped to colour Andrea’s own decisions when she was met with her diagnosis. After the mother of two found a lump in February 2018, she consulted, Dr. Heather Austin, her family physician. … View full news story.
Meet Melissa and Adrien
“He has a bit of a cough,” the daycare workers said to Melissa Bagnall when she picked up her 18 month old son, Adrien. After a restless night, the cough appeared worse and Adrien did not seem like himself. Melissa called the office of her family physician, Dr. Sharpe, for an appointment; they fit them in that afternoon. After seeing how hard Adrien was working to breathe, they were sent to the Maternal Child Care Unit (MCCU) at Prince County Hospital for a consult with Dr. David Wong. When they arrived at the hospital, they were met by Adrien’s father, Glenn. When patients arrive at the hospital unit to see the doctor, pediatric nurses must demonstrate a calm skill-set as they assess, prioritize and manage patients until a doctor arrives. Jaime Richard and Erica Waite were the RNs on duty in MCCU that day. They quickly realized how sick Adrien was and contacted Dr. Wong. A portable chest x-ray revealed that his upper airways were very swollen and becoming so tight that he was using all of the muscles in his chest and belly to suck in each breath. Bloodwork showed that his little lungs were beginning to shut down … View full news story.

“It was a life changing experience. ” – Tyler Kember
September 7, 2019
“It started with a sore throat and ear infection …that’s what I thought it was. It got pretty bad. When I couldn’t keep any water down, I went to PCH Emergency – waited, had a brief exam and was sent home because it was thought to be viral,” said Tyler Kember in a spring 2019 interview. The Summerside business owner and father of three was presenting with what seemed like common cold and flu symptoms. “I went to see my family doctor on Monday and he called PCH and sent me to Emergency. There was a stretcher waiting. My doctor later told me that in another four hours I could have been dead. I was one of the sickest people he’d ever had in the medical centre.” “My kidneys had shut down and I was septic – they didn’t really know the cause of it. If my blood hadn’t been infected – it just looked like normal stuff (the previous symptoms). By then I had a pretty big swelling on my neck. They monitored me to try to figure what it was. At first they thought it might be strep throat and they might need to do surgery. I couldn’t … View full news story.
Cardiac Care Close to Home : Angie MacCaull
May 6, 2019
“I just wanted to be home.” This was not the sentiment Angie MacCaull and her husband Mike were hoping for when they set out for a cruise out of Miami. They would never set foot on the boat. Angie was doubled over in pain in her Florida hotel room when they decided to rush back to PEI for treatment. With the severe heaviness in her chest, they knew it was something serious. In the lead up to the trip, Angie had endured similar attacks. Having ruled out a number of possibilities including a gallbladder issue, through blood work, ultrasounds, electrocardiographs (ECG) and other testing at PCH, she was released with what was thought to be acid reflux. The attending physician encouraged her to return if she had further pain. “It was the best thing he could have said to me,” she remarked. Upon arrival home, Angie was admitted to PCH for extensive testing. By the next day, it was suggested that a family history of esophageal spasms could be the culprit and she was medicated accordingly. The treatment appeared to be working, and she was able to go home. The attacks returned that night and Angie went back to … View full news story.
Meet the Handrahans – Grateful for Care
May 16, 2018
There are no planned accidents. You never know when an accident will happen. But, when Bernard and Sharon Handrahan were in a car accident this February, the team at Prince County Hospital was ready and fully equipped to help them. Though it was a “write off,” their van and its air bags kept them alive despite hitting a tree so hard that their headlights were now facing each other. “We hit it right in the middle,” said Bernard in a recent PCH Foundation interview. “If it had been more right or left, there’d only be one of us here. I was stunned. I knew Sharon was hurt, but I couldn’t move. I couldn’t even check if she was okay.” Sharon was not, in fact, okay. The couple from Christopher’s Cross (just outside of Tignish) was rushed to the PCH Emergency Department. Through Digital Radiography (x-rays) and numerous other tests, it was a determined Sharon had several fractured ribs, as well as a collapsed lung and would need emergency surgery. “It was amazing,” she said. “Before I knew it, they had diagnosed me. You get to see them all work and it’s a well-oiled machine. They all have their jobs … View full news story.
Refitting the ORs
May 30, 2017
“It is unimaginable to think what our story would be if these services were not available at the PCH.” That is the sentiment Lori Pomeroy expressed when she discussed the life saving surgery her son Campbell received at the Prince County Hospital two years ago. He was rushed to the Emergency Department at the PCH with what the family thought were flu-like symptoms that were persisting for days. However, Campbell’s body was quickly “shutting down” and he required emergency surgery. While in surgery, it was discovered that his bowel had twisted and ruptured and he was septic. It was determined he had Meckel’s Diverticulum and consequently he had 60cm of his small intestine removed that day. “It was a very intense situation and doctors told us ideally he would be airlifted to IWK,” says Lori. “However, he was not stable enough to be transported. He did not have time. So, without the teams in Emergency services, the Operating Room, and the equipment used that day at the PCH, our son would not have made it. We are forever grateful that we can share this miraculous story.” This surgery and many others have been possible because of the team in Surgical … View full news story.
My Personal Care Hospital Gordon MacFarlane
On an ordinary day last winter, Gordon MacFarlane was in Pownal at a hockey tournament with his son, Matt. Before lunch he began to feel an all too familiar nausea, followed by intense pain. Leaving his son with another parent he began to make his way to Prince County Hospital (PCH). He called his mother in Stanley Bridge, saying he didn’t think he could make it home and would come there. He coasted into his mother’s driveway where she would find him slumped over the wheel of his car. She called an ambulance and he was rushed to PCH. Over the years, Gordon has had numerous surgeries as a result of the ulcerative colitis he’s had since age 15. The condition is an inflammatory bowel disease that causes long-lasting inflammation and ulcers and led to the removal of Gordon’s lower intestine over the course of two operations in 2003 and 2007 and replaced by stretching and expanding his small intestine. Those surgeries, coupled with a liver transplant performed in 2005, means that Gordon has significant scar tissue in his abdomen, strands of which occasionally attach to his small intestine, kinking it. The liver transplant has also meant a number of … View full news story.
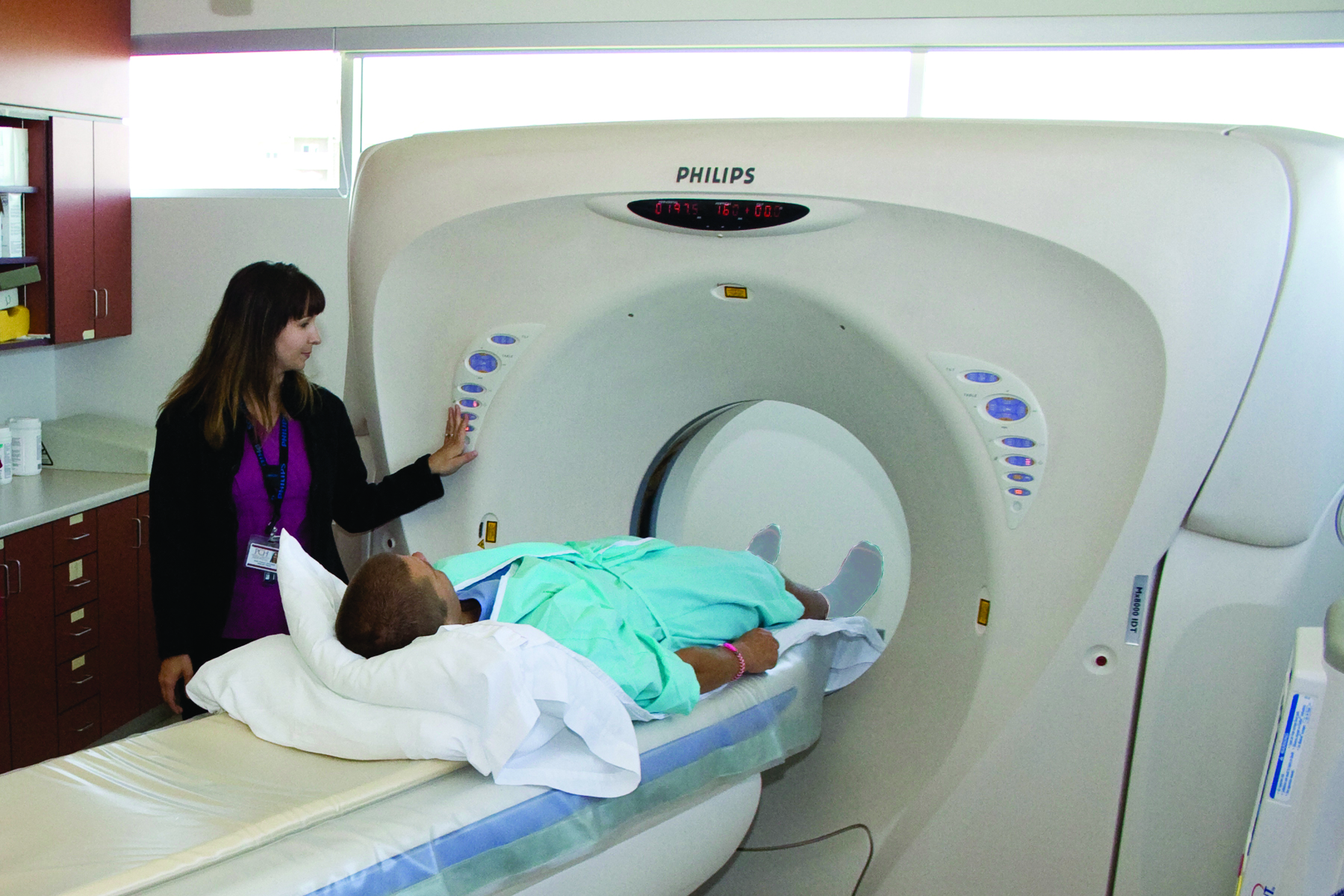
Mendoza Family – Our Personal Care Hospital
For the Mendoza family, PCH doesn’t just stand for Prince County Hospital – for them it has become the Personal Care Hospital. Since Mitchell (20) was diagnosed with Crohn’s disease in 2006, they have become family at PCH. When they walk into the Emergency Department or the Maternal Child Care Unit, they are instantly recognized. Over the years this chronic disease has led Mitchell through PCH for treatment and testing in the ever-growing need to understand and combat this disease. Whether receiving testing in the laboratory, being admitted for pain through Emergency, receiving a scope or an iron infusion in the Endoscopy service of Ambulatory Care, or spending time in Paediatrics, Mitchell has become accustomed to the hallways of his personal care hospital. It is this personal care received from their PCH family that has carried the Mendoza family through tough times over the years. Mitchell beams as he talks of care close to home and how it is truly his community caring for him. “We knew 6 nurses personally when I was first admitted. I knew 3 of my nurses in my surgery and even my family doctor scrubbed in just to make sure everything went alright. My next … View full news story.

Anna Smith – How I Spent My March Break
How I Spent My March Break – with Anna Smith Over the course of two months, ten-year-old Anna Smith developed what was thought to be a mole that didn’t seem abnormal, but became increasingly annoying. One Sunday she noticed a hard ball under the spot on her left arm. By Wednesday there was a dime-sized red circle around the spot. By the following day it had grown to the size of a toonie and had become a great concern to both her and her mother Lisa. “It really bugged me,” Anna explained. “I didn’t know what it was.” That evening, Anna and her mother made a trip to the Emergency Department (ED) at PCH. The spot was diagnosed as an infection and an antibiotic was prescribed to clear it up. In the case of Anna’s infection, an abscess was evident from the appearance of the skin and the feel of the area, but the first round of antibiotics were ineffective, as was a second antibiotic and the infection continued to spread. With the infection still growing aggressively, Anna and her mother returned to the ED and were seen by Dr. Steven MacNeill who diagnosed the infection as cellulitis. Dr. MacNeill, … View full news story.

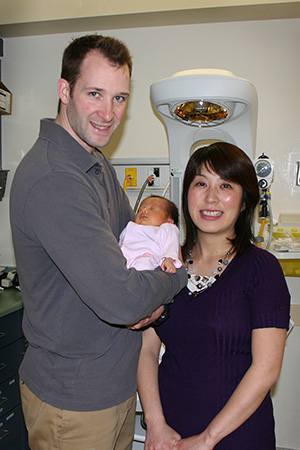
The Hockin Family, Grateful for Quality Care
Nao Hockin was aware that she would be delivering her baby earlier than usual. She was admitted to PCH on Wednesday, February 20th and at 36 weeks Nao’s labour was induced. She was in mild labour throughout the day, however that all intensified when her water broke at 5:00 pm. Baby girl Rina Hockin was born February 21st at 1:39 am. She was 4 weeks early and weighed 4 lbs, 2 ozs. Due to her early arrival, Tim and Nao did not know what complications may arise or if their baby would be able to breathe on her own. With a room full of healthcare professionals including Dr. Freeman, Dr. Farag, Respiratory Therapist Abdul Rahma and Nursing staff, the Panda iRes Infant Warmer was prepared. This new technology was imperative in baby Rina’s first moments. The unit provides the necessary warmth but also had the ability to measure her oxygen saturation. Fortunately, PCH was equipped with the Infant Warmers as the Foundation recently purchased two units in 2012 thanks to the generous donations received from the community. “She was so small that she was not able to maintain her body heat,” says new father Tim Hockin, “but luckily she was … View full news story.